 Recurrent miscarriage may be associated with MTHFR.
Recurrent miscarriage may be associated with MTHFR.
Yet, many health professionals dismiss this heavily researched association.
Does this sound familiar: “I was just told by my high-risk OB that there is no research proving MTHFR is connected to miscarriage.”
If this does sound familiar, your OB is not educated correctly about MTHFR.
Let me give you something which will disprove the naysayers immediately.
This image below comes straight from the CDC (Centers for Disease Control AND Prevention)
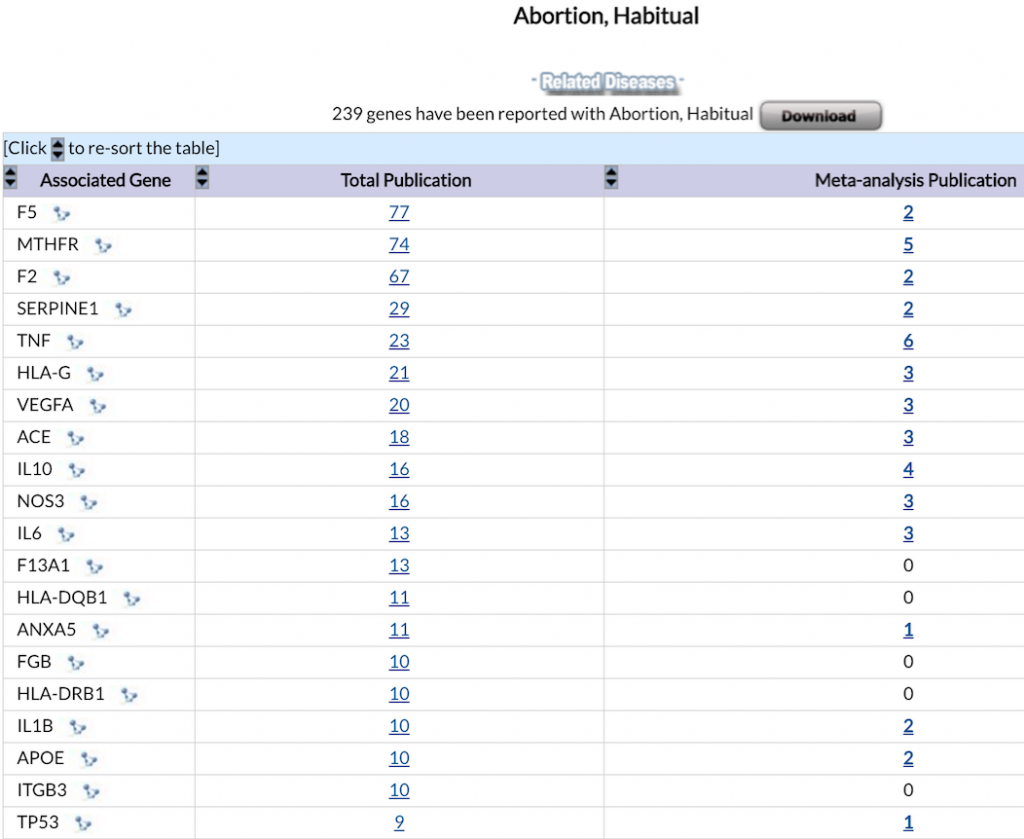
source: CDC Phenopedia
The #1 gene associated with recurrent miscarriage is Factor V Leiden (F5).
This is known and accepted in medicine.
What is the #2 most researched gene associated with recurrent miscarriage?
MTHFR with 74 research papers and 5 meta-analyses.
There is conflicting evidence. Yes. Some papers say MTHFR is associated with recurrent miscarriage and others say it is not.
“Several case-control studies were investigated MTHFR C677T polymorphism as risk for recurrent pregnancy loss (RPL). These studies rendered contradictory results, some indicating that the polymorphism is associated with the risk of RPL whereas others concluded there is no association.”
Why are there contradictory results?
Because some women with MTHFR polymorphisms consume leafy green vegetables, limit folic acid intake and have their methylation cycle working well.
Some women with MTHFR polymorphisms have a different story and life experience and their methylation cycle is not working well.
It depends.
Just because you have a MTHFR polymorphism does not automatically say you are going to have recurrent miscarriages.
What having the MTHFR polymorphism does say is you have an increased risk for recurrent miscarriages.
For years, since 2011, I have been teaching and educating many people around the world about MTHFR.
How many times do you think I’ve heard this?
“Just had my OB tell me MTHFR is a variant akin to having eye color and everyone’s eye color is different and there is no need to do any kind of treatment . Big eye roll. I lost 6 pregnancies and since taking methylated B’s I’ve had 3 back to back pregnancies.”
This is the most thorough article on MTHFR and Pregnancy out there. Read this article thoroughly along with taking action on the resources I recommend.
I’ve heard it a ton.
Summary:
- If you are having recurrent miscarriages, you seriously need to consider doing genetic testing with your doctor. Check for F5 and MTHFR for starters.
- If you have NOT yet ordered genetic testing, consider StrateGene DNA Test – I no longer recommended 23andme.
- Already ordered genetic testing from 23andMe or AncestryDNA? Consider getting more comprehensive information by using StrateGene to point out additional polymorphisms.
- Remove folic acid and start using more active forms of nutrients which your body – and your baby – can efficiently use.
- Learn. The. Science. A great informational video is here on ‘Folic acid and Pregnancy’ – along with over 353 brilliant comments posted by readers.





Q: hetero C677T; 8 miscarriages. 2 live births using low dose aspirin. Knowing that MTHFR miscarriages are often an issue with artheriosclerosis of the umbilical cord, do you think I should probably be on low dose aspirin now that I’m in my late 40’s, to head off heart issues?
I miscarried 2 put of 4 pregnancies. I have two sets of MTHFR
Hi Dr.Lynch my mother had the MTHFR gene & doctors don’t know what to do with her but to put her on all different kinds of medication. It really saddens me because she wants to get better & it seems like she’s not. It’s been two years now and no one “knows what wrong with her” besides that she had this gene.
Sorry to hear this.
There are many great organizations to find quality health professionals. http://www.seekinghealth.org and http://www.naturopathic.org and http://www.functionalmedicine.org – those are where she needs to find a great health professional.
Taylor- naturopaths usually have a doctorate in biochemistry, more biochemistry than MDs and Pharmacists. My Dad had a PhD in neuropharmacology, and my naturopath had more of a background than my Dad, and could answer questions my Dad couldn’t. If you are looking for someone who knows how to read labs, rather than just tell you everything looks “normal” call on. Naturopath.
I have MTHFR C677T and so does my husband. I am taking all the supplements in your prenatal/pregnancy protocol since my 2nd and last miscarriage in 10/2016. And I have been secretly putting seeking health multivitamin powder in my husbands shakes 😉 I’d like to know if you know about WOBENZYME and if you would recommend to take as substitute to baby aspirin while TTC and during pregnancy? I do not know if I have blood clots or high homocysteine levels. Our doctors do not take MTHFR seriously the most they recommend is take a stronger prenatal that has both folic acid AND Quatrefolic® . Will we do just fine with taking your prenatal supplement recommendations and nothing else? I just turned 41 and getting older (biologically).
Hi Isabel – great question. I am not sure if Wobenzyme is safe during pregnancy. I’d think not but not sure.
I’d consider the:
– Optimal PC
– Optimal Fish Oil
– Vitamin D
– ProBiota 12
– Optimal Liposomal Vitamin C
– Optimal Liposomal Glutathione until pregnant and then stop
Sure would like you to check your homocysteine levels. Please find a doctor who will.
If your homocysteine is higher, then you would need to supplement with more nutrients – possibly HomocysteX Plus in addition to the prenatal.
Hi Dr. Lynch. Thank you for this informative website. I’m wondering if you would give me some recommendations for what supplements to take? I have two MTHFR gene mutations, C677T and A1298C (both heterozygous). My homocysteine level is 5.3. I’m currently taking a prenatal vitamin with folate as L-5-Methyltetrahydrofolate. Also the B6 as Pyridoxal 5′-Phosphate and B12 as Methylcobalamin. Thanks for your time and help.
Hi Dr. Lynch,
After telling our fertility doctor that I am compound heterozygous for MTHFR, he said that most of the population has an MTHFR diagnosis & its no big deal. Then told me to take more folic acid. My (simplified) understanding from reading here on your site, is that Folic Acid is the synthetic form of Folate & should be avoided. What I need more of is folate. Is this correct?
Our currrent doctor also plans to put me on birth control for a short period of time while we go through the procedures of IVF, to help regulate my cycle. My reading has informed me that BC can deplete those with MTHFR folate & other vital nutrients.
I’m thinking I should find a doctor who specializes in both Fertility & MTHFR. Do you know of anyone who works in the San Francisco area?
Do you have any specific advice for me or someone like me?
Thank you,
Hi Evelyn –
You’re right. Nailed it actually.
Please watch the video on this page and also read the text. The video will provide a lot of information for you. https://mthfr.net/prenatal-supplementation-optimizing-your-future-child/2012/01/20/
Hi Dr. Lynch,
Thank you so much for posting your research. I’ve had 5 RPL since last October. I am 41, first child, and feel like I’m at the end of the road with this journey. After expensive surgeries, and unthorough testing, I finally found a doctor that sent me for genetic testing and discovered I’m an MTHFR homozygous mutant! I felt so confident that after 5 doctor’s I finally found one that can help us, then when I asked our approach she said to take 5mg of folic acid – just like all of the other fertility specialists and obgyns that I’ve seen. This is very concerning for me after all the research I’ve done on the internet regarding the issue. I still don’t even know if it is MTHFR mutation that is causing the miscarriages. They have all terminated between 5-6 weeks. I’ve started taking 1mg of 5-meth this week and really looking forward for relief of life long ailments associated by this gene mutation. I’m from Seattle i think like you, but I live in another country that speaks a language I’m not yet fluent, so that brings on its own set of obstacles. Do you do online consultations? Or are there any factors that I should look at further investigating?
Thank you again!
Hi Mariposa
I have had similar issues to what you have described. The solution for me was being put on metformin. I don’t know if it would work for you, I was advised of this before I knew I had a homozygous MTHFR issue. I went to a specialist at an IVF clinic (didn’t need IVF). He put me on this and bang, I stopped miscarrying. Since my son was born 4 years ago, I had been wanting to try again but delayed matters for 12 months on learning of my MTHFR issues and beginning a regime of supplementation for methylation etc. I was hopeful I wouldn’t miscarry again and didn’t use metformin. I just miscarried again last week so will be going back on Metformin as well. I queried Dr Lynch about this and he suggested that this was ok to do with appropriate B12 supplementation. You can find my query and his answer if you look at his metformin article. I am now 43 and pretty upset I waited so long trying to improve my methylation. Hopefully with now having metformin on board again everything will work but I know it isn’t a guarantee. At least with the supplementation, hopefully I have more chance of a healthy baby if I get so far as keeping one. I wish you well xx
I suffered a complete and concealed, placental abruption (22 weeks, fetal demise). My placental pathology showed it began growing very badly which lead to the abruption. I was tested for all blood clotting disorders, all negative. I did my own research and found MTHRF as a potential risk factor. Again, I had no known causes for Placental Abruption aside from the clotting. ie: nonsmoker, no drug use, no trauma etc.
At my first MFM appointment post stillbirth, I asked about this gene mutation. She dismissed it within 3 seconds and said they are not connected. How do I seek to be tested for this and if I have it, is there a recourse for a second pregnancy? My MFM only has me set up to take baby aspirin during my next pregnancy.
I currently take and took, Prenate Mini which has folic acide not folate. I do not know if I have this gene mutation but really want to be tested if you would believe it could be connected to my abruption.
Dr Lynch
I’m so appreciative of you work. I had 3 miscarriages in my early 20s, one at 12 weeks after we had heard the heartbeat, we had genetic testing done on the baby and found no chromosomal abnormalities. After lots of research I was convinced I had Factor V, but after working with a mainstream fertility doctor I tested negative. But blood clotting was the only cause that made sense to me. Being health conscious I only ever took folate, never folic acid. I began cleaning up what I ate, reducing folic acid from enriched grains, because I changed to a paleo diet. I conceived and had a healthy boy. Then 2 years later I had another miscarriage. Then I got pregnant again and my midwife referred me to your research, I am hetro A1298c. I started your recommended supplements (and a few weeks on baby asprin). Just a few weeks ago had a healthy baby girl.
My question is what future supplementation should I be taking to prevent heart issues?
Should/when should I have my children tested for MTHFR? They are ages 3 year and 7 weeks.
Once again I am so thankful for your work. Thanks to your work I might be able to avoid the pain and loss of anther miscarriage, and I am truly grateful.
McKenzie
I have a single copy of c667t and have a question about nattokinase. Instead of taking a supplement could I simply eat natto? Any thoughts on how much natto I would need to eat daily? I currently eat about 1oz of organic natto per day. A little background on me; I’ve have three children with three miscarriages (at 8-11 weeks) between each with the last being a lost twin. I’m currently pregnant but am not optimistic. Im following a nutritional balancing protocol as well as many of your recommendations as well.
Thank you!
I am Homozygous C677T and after two recurrent miscarriages I am taking the Optimal Prenatals, Optimal PC, Optimal Fish Oil, Vitamin D, Probiota 12 and two lozenges of Active B12 with L-5 MTHF daily; should I take a daily baby aspirin as well?
Hi Dr. Lynch,
I have both C677T and A1298C, I have one toddler and then last year lost a baby at 22 weeks and then had a miscarriage. I ordered the optimal prenatal but since I live in Mexico turns out it got detained in customs and couldn’t be delivered. I already had it rerouted to an address in the US but I can’t pick it up until at least one month from now.
So my question is what can I do meanwhile? I have not been able to find any prenatal here that does not contain folic acid. I have increased my intake of leafy greens and beans and have started eating lentils. I’m doctor also has me on baby aspirin. Could this be good enough for now?
It is still too early to test but I have a feeling I may already be pregnant again.
Hi Dr. Lynch,
Thanks for all the great information! I have just discovered that I am homozygous for C677T, after two back to back miscarriages. I have since cut all synthetic forms of folic acid and started supplementing methyl folate and methyl B12. My diet is extremely clean and I work out 5-6 days a week as well as doing detox (Epsom salt) baths a few times a week. I am having a hard time finding out how long I have to let my body detox and heal before we start trying for another baby… Do you have any advice? Thank you so much!
Hi Dr. Lynch,
Thank you for the informative video and website! I am homozygote C677T. But my homocysteine level comes back low around 2.5. Does that mean I have no problem turning folic acid into folate? I am currently taking Rainbow light prenatal with 800mcg regular folic acid, and I just bought 1mg L-5-methryl from Thorne. Can I still take the regular prenatal?
How much folate should I take daily?
Please read and watch this video –
taking folic acid is not a good idea during pregnancy.
taking folate is.
https://mthfr.net/prenatal-supplementation-optimizing-your-future-child/2012/01/20/
Low homocysteine is a sign that:
– may be not eating or absorbing enough protein
– higher oxidative stress and pushing production of glutathione (using up homocysteine)
Both of those need to be evaluated and homocysteine needs to be raised to about 7 or 8.
For anyone who has had recurrent miscarriage, I had 5 miscarriages in a row before the recent birth of our daughter. I have written an article about how I treated myself mostly through changes to my diet. Here is the link to my first post in the series.
http://www.homeschoolbuilt.com/pregnancy-after-recurrent-miscarriage-introduction/
I just came across this resource, and I am so thankful for it. I have now had 3 recurrent miscarriages following the same exact pattern: confirmed heartbeat at 6 weeks and miscarriage roughly 2-3 days later. My OB & MFM knew I have MTHFR (homozygous) and assured me 4 grams of folic acid/day and a baby aspirin were all I needed for a healthy pregnancy. They assured me MTHFR was as common a genetic deviation as freckles and needed no special diet or supplementation. Based upon your research, they couldn’t have been more misinformed. I am so thankful for the research you’ve put together. It’s given us hope for a family in the future.
I must be lucky. My ob/gyn said to me…. With your history of premature births and miscarriages I almost guarantee you have MTHFR. My father has it and so I asked about it. I do have it Homozygous type as does my father.
Hi Bonnie –
MTHFR does increase risk – but it can definitely be reduced significantly. Please read this article on MTHFR and pregnancy. I’ve worked with many clients who had recurrent miscarriage and they had a successful pregnancy and beautiful healthy child. You can too! 🙂
Hi Dr. Lynch,
I’ve been reading a lot about the methylation process lately. I miscarried my first pregnancy which let me to do 23 and me where I learned I am hetero A1298C with normal CC677T and Homozygous MAO A with normal COMT. I switched my prenatal after miscarrying for one that included 1.13mg L-methyl-folate (as Metafolin) which gave the worst anxiety I’ve ever experienced in my life. I’ve read a lot about how MAO A and folate don’t get a long. Your prenatal looks great, but given my previous experience with Folate it scares me a little. If I understand correctly this is a different type of folate than the one I took before, is that correct?
Hi Carla –
I am glad you are looking into a better formulated prenatal.
Optimal Prenatal uses a combination of folate – folinic acid (400 mcg) and MTHF (400 mcg)
Pregnancy requires both forms of folate – not just methylfolate.
Please read this article on pregnancy, MTHFR and supplementation.
I highly recommend the Optimal Prenatal Protein Powder – vanilla is my preferred flavor. You can actually use the capsules, powder and chewables – and rotate them as you desire. Some days have the smoothie, other days capsules and other days the chewable.
1.13 mg of MTHF is a lot – you are correct.
It is FAR from all you need for pregnancy as well.
This is a very educational opportunity also on how to have a great pregnancy
i had 3 misscarriages and after the 2nd a blood clot was suspected to have traveled to the baby when no heartbeat was heard on week 11. Blood clotting disorder was suspected i advocated and demanded to be sent for testing by perinatologist. I found i have mthfr both genes. Started baby aspirin and prenatals got a new ob who knew about mthfr and said when i would get pregnant again he would start me on lovenox injections daily i did this from 5 weeks on and today i have a beautiful 4 year old thank you dr jason lowe and lovenox! Another tip ive found out ive suffered from major depression and anxiety since 12 years old possibly also linked to mthfr through research i found out about a pharmaceautical food called deplin that can be added to your antidepressant i asked my psychiatrist about mthfr he knows about it i told him i had it and he said he had samples and was putting me on the deplin from day 1 i feel like a new person my depression has lifted i hardly take my anxiety meds im happy im so greatful if you have mthfr and mental illness get on deplin asap it has changed my life.
Hello, I had 4 miscarriages and 4 live births. I have both mthfr genes. My mom had 2 miscarriages and 2 live births. My youngest daughter had 4 miscarriages no live births. I know she received one mthfr gene from me. I truly believe this is why I had miscarried. I have so many health problems that I believe are do to MTHFR.
Dr. Lynch,
I had 3 successful pregnancies followed by 3 miscarriages (15 weeks, 5 weeks, 13 weeks). Blood work confirmed homozygous c677t & low thyroid. I have started supplementing methylfolate, d3, prenatal & b12. How do I know if I need to be on baby aspirin or something similar?
Hello Dr. Lynch,
I had 2 miscarriages. All standard tests were normal. I have C677T mutation homozygous. My sister has done mutation heterozygous and has a child with spina bifida myelomenigocele. Can you recommend a doctor in the midwest who deals with MTHFR mutations?
Hi Ben,
What are your thoughts on low-dose aspirin to prevent miscarriage (one miscarriage, one copy A1298C)?
Thank you!
Hi Emily –
Baby aspirin or low dose has definitely helped some women prevent miscarriage. One may look at other alternatives like fish oil, vitamin K2, cleaning up their NOS3 gene (as discussed in my book, Dirty Genes)
God freaking darn it! I am in my 40s and reading this website because I’m trying to understand why the B complex I take for my arthritis has magically and instantly cured my lifelong depression. Glad I finally found out about this. But it would have been nice to have some doctor somewhere get off his butt and do a little research. Especially during the years when I had SEVEN MISCARRIAGES and the OBGYN just told me it was bad luck and keep trying.
Hi Dr. Lynch
I’ve had 7 recurrent loses. I am homozygous C677T and have Factor 5 i was curious as all my OB n hematologist say my Folbic isn’t causing my losses but i think different . I do have 1 child ( was 26 )before i found all this out when i hit 30.
Just wondering if there is anything i can be doing different!?
Thanks
I’ve recently found out that I have two copies (homozygous) of MTHFR c.1286A >C. However, I’ve been told this is of little clinical significance. I’ve had three recurrent miscarriages so I wanted to see what your thoughts on this are. Thanks!
Hi Caoimhe – that is not insignificant. It reduces your MTHFR enzyme by about 40% but do keep in mind there there may be other SNPs that are significant – like NOS3, COMT, DAO, TNF, BCO1, etc –
Ru your 23andme and Ancestry data through StrateGene to see this information.
Hi Dr. Lynch, I recently had a miscarriage and discovered i am homozygous A1298C mutation. I started taking your prenatals about a month ago, what is the period of time that I need to wait before trying to get pregnant again? Do I need to wait for an adjustment period?
Thank you in advance!
Rose from Buffalo NY
Hi Rose –
Ideally anywhere from 3 to 6 months. It’s not just about taking the right prenatal but also diet, lifestyle, gut health, etc. Please read this article on MTHFR and Pregnancy
I have had 2 still births. The first was a 22 weeks and second was at 24 weeks. The doctors have not been able to give me any reason why this happened. Chromosomes were tested and everything was negative. I had an amniocentesis that checked for genetic disorders and infection. All negative. I was just tested fro the MTHFR gene mutation and came back with heterozygous A1298C mutation. Everything i have read has not listed that mutation as being one to cause miscarriage. Am i wrong about this? Im just hoping for an answer and some way to have a healthy baby. Will added the B supplements help?
Hi Ashley – I’m sorry about your still births.
Please read this ‘how to use prenatal vitamins‘ article for an optimal pregnancy
Hi dr Lynch! Few weeks after I got birth to a beautifull dauther, I had found out that I did a postnatal complication: deep vein trombosys and embolism. My cardiolog sent me to do some genetic testing and I found out that I have factor V Leiden, MTHFR -1298 hetero, and PAI genotip GG. What should I do for next time when I want to have another baby?
Hi Ramona –
There is a lot of things to do to help reduce clotting risk. Please read and follow recommendations here on MTHFR and Pregnancy.
You’ll also likely need to be put on Lovenox. Talk with your doctor about this.
I have 4 live children that I am very thankful for but going through my 3rd miscarriage right now. My father and daughter both tested positive for MTHFR mutations so children and I are only allowing methyl b-vitamins to enter our bodies. Thank you for all the additional information of what is necessary for a healthy and successful pregnancy. I’m curious if I should try to get my husband to try to take methyl b-vitamins and any other supplements would that help?
Hi Rachel –
I’m happy you are learning how to optimize future pregnancies. That’s huge.
You absolutely should have your husband also take these methylated nutrients – or at least some type of quality multivitamin.
This is a very informative article on MTHFR and pregnancy for you both – and after you read it fully – you’ll have a lot more information to take action with. I highly recommend the Optimal Prenatal with Plant Based Protein – for both of you. You can easily add 1.5 or 2 scoops in your smoothie in the mornings and you both then have your vitamins and your breakfast 😉
Doctor Ben .. i have 2 misscariages my blood test shows heterozygote for mthfr 667 my doctor said there is no relation .. i took many info from this video but i want to make sure this mutation is really the cause
I have my new artificial insemenation next month plz i want to know what shoukd i do . Start taking baby spirin folate and b6 and b12 from now
Hi Rawan –
Here you go – this is what you need to read on pregnancy and MTHFR and apply right away.
Hi Rawan –
I don’t think your MTHFR variant is the cause of your recurrent miscarriages. What I think could be contributing though is related to how MTHFR impacts methylation. Often times, methylation dysfunction is what contributes to recurrent miscarriages – but not always. There are also clotting disorders like PA-1, NOS3 and F5 which are very common and problematic.
Definitely apply what you learned in the video – it will help. You may also need to be put on Lovenox. Need to check your homocysteine levels and also clotting scores.
Hi! I have a healthy 2 year old but have been trying for second for 21 mo and had 2 miscarriages at 6-7 weeks both missed miscarriages. I have since found out I have heterozygous c677t mthfr and heterozygous factor v Leiden. I may try again with iui next month and dr has plans for lovenox and antihistamine protocol. Homocysteine was 5.8 so they don’t think it was mthfr. Nevertheless I’m following you advice in dirty genes for mthfr. Is there anything I can do for factor v Leiden?
Hi Brittany –
I highly recommend you use Optimal Prenatal with Plant Based Protein – vanilla. You need the additional protein it provides and the additional specialty ingredients.
There is no better prenatal available and you need the best support possible.
For FVL, I’d add in Lovenox – talk with your doctor. You may also want to use Baby Aspirin in the interim until this happens.
Do consider everything I discuss here in the article on MTHFR and Pregnancy – even if you don’t have MTHFR, it’s important to apply all of these and I explain why.
A low homocysteine doesn’t mean you don’t have a MTHFR variant. It may mean you have low glutathione, poor protein absorption or low intake of protein.
Hi Dr. Lynch, Are you concerned about the research suggesting that excessively high levels of B12 and folate in prenatal vitamins can increase the chances of having children with Autism?
1,875% of B12 in your pre-natal, seems really high, is it not?
I just had a miscarriage and am homozygous MTHFR A1298C. Looking for a prenatal regimen that will better support this mutation, but I feel so confused by all the conflicting information!
Appreciate any feedback!
Hi Kristin –
There is a lot of conflicting information.
The issue is because people are not looking at the whole picture. If we focus on single variables, then problems won’t be solved.
High B12 and/or high folate is not the problem for increasing autism risk.
The high B12 and/or high folate found in the study associated with increased risk of autism is missing a bigger picture.
B12 and folate are found in the blood in lab tests.
B12 and folate are supposed to be inside the cell – and used there.
The issue is people with high B12 and high folate are not getting these out of their blood and into their cells.
It’s stuck.
This is due to low glutathione, heavy metals, inflammation and the wrong forms of folate and B12.
That’s the issue.
These are all risk factors for increasing autism.
So the high B12 and high folate are not the causative factors. They are what is initially seen.
One has to dig deeper.
Researchers are not digging deep enough.
Read this article on MTHFR and pregnancy. It will help you immensely. 😉